Epilepsy (मिरगी)
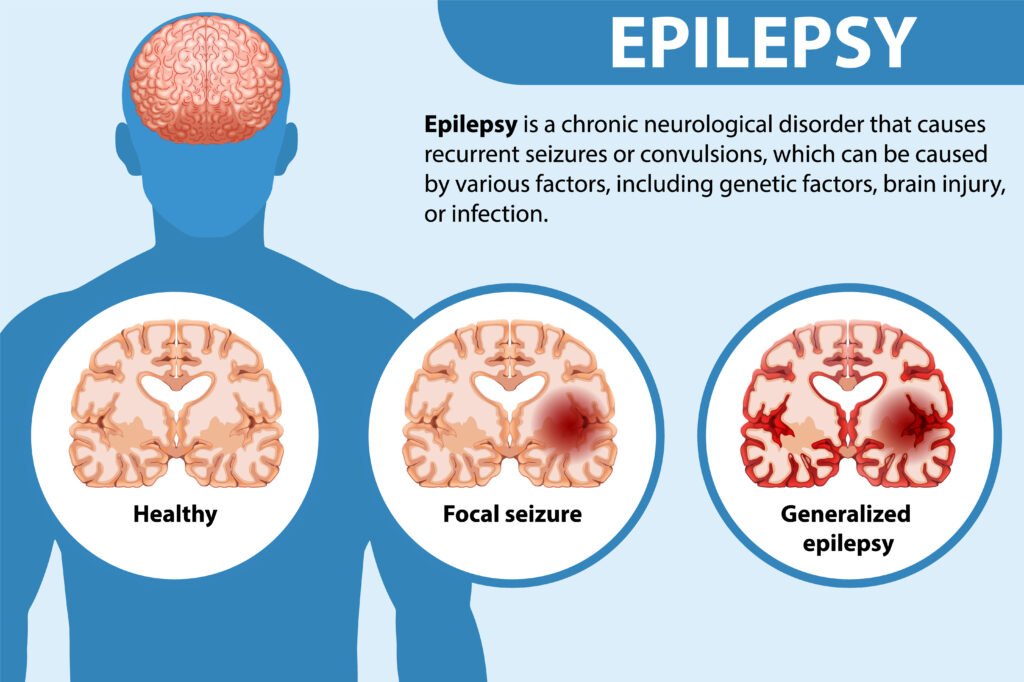
Epilepsy is a chronic neurological disorder characterized by recurrent seizures—sudden bursts of electrical activity in the brain that can cause changes in behavior, sensations, or consciousness. As your neurologist, I aim to explain epilepsy in clear, compassionate terms, outline how we diagnose and treat it, and share practical tips for living well.
What Is Epilepsy?
Epilepsy affects an estimated 50 million people worldwide. A single seizure does not constitute epilepsy; it is defined by having two or more unprovoked seizures. Seizures arise when clusters of nerve cells fire abnormally, leading to anything from a brief lapse in attention to full-body convulsions (World Health Organization).
Common Seizure Types
Generalized tonic-clonic: Stiffening followed by rhythmic jerking of limbs.
Focal aware: Jerks, tingling, or visual disturbances in one part of the body while consciousness is preserved.
Focal impaired awareness: Confusion, staring spells, or repetitive movements with reduced awareness.
Absence seizures: Brief staring episodes, often mistaken for daydreaming.
Recognizing the Signs
Key symptoms that warrant evaluation include:
Sudden, unexplained jerking movements or loss of awareness
Unusual sensations (tingling, smells, tastes) before a seizure
Confusion or loss of memory following episodes
Injuries sustained during seizures
Early recognition and prompt assessment enable timely intervention, improving outcomes.
How We Diagnose Epilepsy
Detailed History & Exam: I’ll review your seizure descriptions, triggers, and overall health.
Electroencephalogram (EEG): Records brain waves to detect abnormal patterns even between seizures (Mayo Clinic).
Brain Imaging: MRI or CT scans to rule out tumors, vascular lesions, or structural abnormalities.
Blood Tests: Identify metabolic, infectious, or genetic factors contributing to seizures.
Together, these tools help determine seizure type and guide personalized treatment plans.
Treatment Approaches
While most people achieve good seizure control, about one-third develop refractory epilepsy. Our treatment goals are seizure freedom with minimal side effects.
1. Anti-Seizure Medications
First-line options include lamotrigine, levetiracetam, and carbamazepine, chosen based on seizure type, age, and comorbidities (WHO).
Medication is started at a low dose and gradually adjusted for optimal control.
Adherence is critical—never stop or change doses without medical guidance.
2. Surgery and Neuromodulation
For drug-resistant focal epilepsy, surgical resection of the seizure focus can be curative.
Vagus nerve stimulation and deep brain stimulation offer non-resective options for patients ineligible for surgery.
3. Dietary Therapy
A medically supervised ketogenic diet (high fat, low carbohydrate) may reduce seizures, particularly in children.
Living Well with Epilepsy
Maintain a seizure diary to track frequency, triggers, and medication effects.
Prioritize adequate sleep, stress management, and hydration—seizure triggers you can control.
Wear a medical alert bracelet and inform friends or colleagues about seizure first-aid steps.
Engage in regular, moderate exercise and follow a balanced diet to support brain health.
When to Seek Help
If you experience new or worsening seizures, medication side effects, or challenges in daily life, please reach out. Early adjustment of your treatment plan can restore stability and confidence.
To schedule your personalized consultation:
Visit our Home Page
I am committed to combining cutting-edge science with genuine empathy, ensuring you and your family feel supported at every step of your epilepsy journey.